 The physiologic changes (fluid shifting from the posterior lung, allowing undamaged alveoli to be filled with oxygenated blood) that occur when turning a patient into a prone position improve ventilation. Turning the patient with ARDS from a supine to a prone position can increase pulmonary capillary perfusion and oxygenation. His facility has an established protocol for prone positioning, which is essential for successful use of this technique. Mark knows that the nurse is responsible for initiating the discussion with the interprofessional critical care team to use this technique to improve oxygenation. Welsh would be a candidate for prone positioning. Welsh is diagnosed with pneumonia, which has contributed to the development of acute respiratory distress syndrome (ARDS). Inotropic therapy with dobutamine at 20 mcg/kg/min is added because of continued hypoperfusion despite achieving a desired MAP. Chest radiography reveals bilateral infiltrates and noncardiac pulmonary edema.Īfter the provider orders vasopressor norepinephrine, titrated to maintain a mean arterial pressure (MAP) of 65 mmHg, Mr. Positive end-expiratory pressure (PEEP) is added to the mechanical ventilator settings in an attempt to avoid alveolar collapse. Aerobic and an aerobic blood cultures are sent to the lab. Mark increases suctioning because of purulent secretions. The fraction of inspired oxygen (FiO 2) percentage can’t be reduced from 100% on the ventilator, and the target tidal volume remains set at 6 mL/kg of predicted body weight to protect lung tissue. 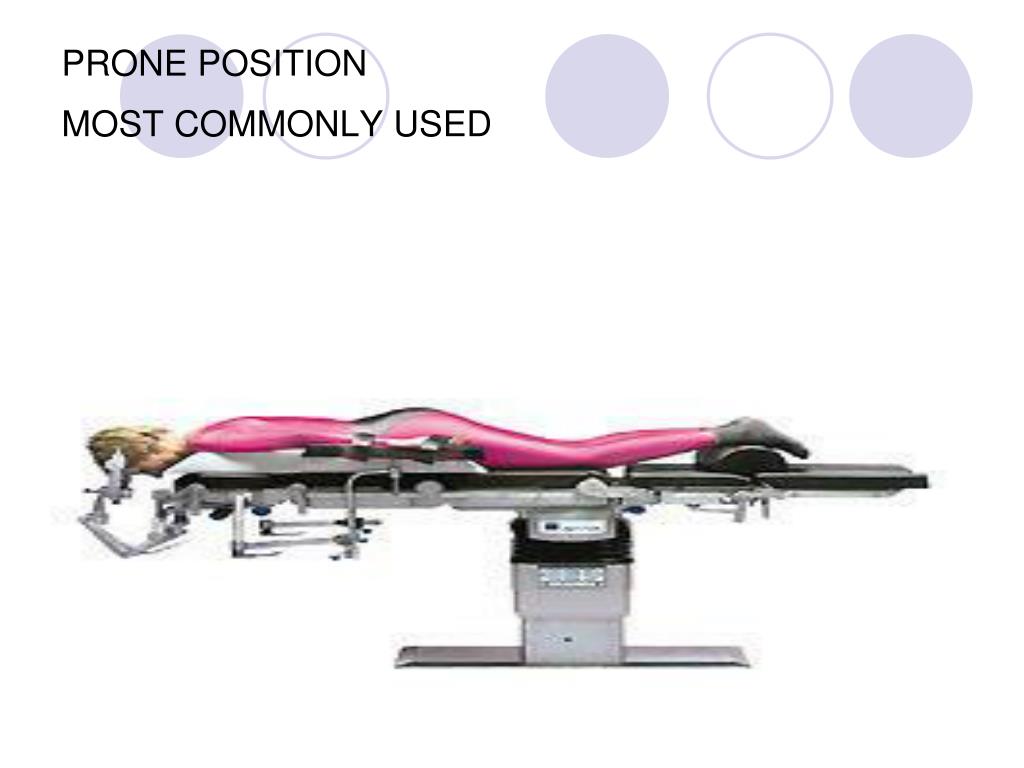
Welsh’s nurse in the ICU, notes that his lab values reveal leukocytosis and respiratory acidosis (pH 7.31, carbon dioxide 48 mEq/L, bicarbonate 24 mEq/L) with hypoxemia and a blood lactate concentration of 5 mmol/L. He’s transferred to the intensive care unit (ICU) for mechanical ventilation. Welsh is more confused and that his blood gases are rapidly deteriorating. The next morning, Sarah, the telemetry unit nurse, observes that Mr. The patient is admitted to the telemetry unit for continued evaluation and treatment of progressive community-acquired pneumonia. Margaret increases the oxygen to a 40% nonrebreather mask, and the provider writes orders for a stat chest X-ray and blood work for arterial blood gas. Welsh’s vital signs are temperature 96.8° F (36° C), apical heart rate (HR) 118 beats per minute (bpm) and regular, respiratory rate (RR) 28 breaths per minute with accessory muscle use, oxygen saturation 87%, and blood pressure (BP) 98/60 mmHg (seated). 
On physical exam, Margaret notes bilateral wheezing and crackles throughout the lower lobes. She applies oxygen at 2 L via nasal cannula. 
Welsh is dyspneic and mildly confused with disorientation to date and time. Welsh, who has type 2 non-insulin dependent diabetes, hasn’t been vaccinated for pneumonia. He reports that he’s been in relatively good health until about a week ago, when he noted a sore throat and “cold symptoms.” He visited his primary care provider, who prescribed azithromycin. He’s experiencing increasing fatigue, fever, chills, and a productive cough. Paul Welsh*, who is 66 years old, is brought to the emergency department (ED) by his family. A coordinated effort of an interprofessional team, trained in a nursing care protocol, can prone positioning an effective and safe intervention.Nursing care of patients in the prone position is challenging, as is the physical act of turning the patient from supine to prone.In patients with moderate to severe ARDS, who are mechanically ventilated, early use of the prone position has increased survival rates.Appropriate use of prone positioning can improve patient outcomes. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
